Acute COVID-19 severity and mental health morbidity trajectories in patient populations
About This Project
Acute COVID-19 severity and mental health morbidity trajectories in patient populations of six nations: an observational study
The Lancet Public Health, doi: 10.1016/S2468-2667(22)00042-1
Summary
Background. Long-term mental and physical health consequences of COVID-19 (long COVID) are a persistent public health concern. Little is still known about the long-term mental health of non-hospitalised patients with COVID-19 with varying illness severities. Our aim was to assess the prevalence of adverse mental health symptoms among individuals diagnosed with COVID-19 in the general population by acute infection severity up to 16 months after diagnosis.
Methods. This observational follow-up study included seven prospectively planned cohorts across six countries (Denmark, Estonia, Iceland, Norway, Sweden, and the UK). Participants were recruited from March 27, 2020, to Aug 13, 2021. Individuals aged 18 years or older were eligible to participate. In a cross-sectional analysis, we contrasted symptom prevalence of depression, anxiety, COVID-19-related distress, and poor sleep quality (screened with validated mental health instruments) among individuals with and without a diagnosis of COVID-19 at entry, 0–16 months from diagnosis. In a cohort analysis, we further used repeated measures to estimate the change in mental health symptoms before and after COVID-19 diagnosis.
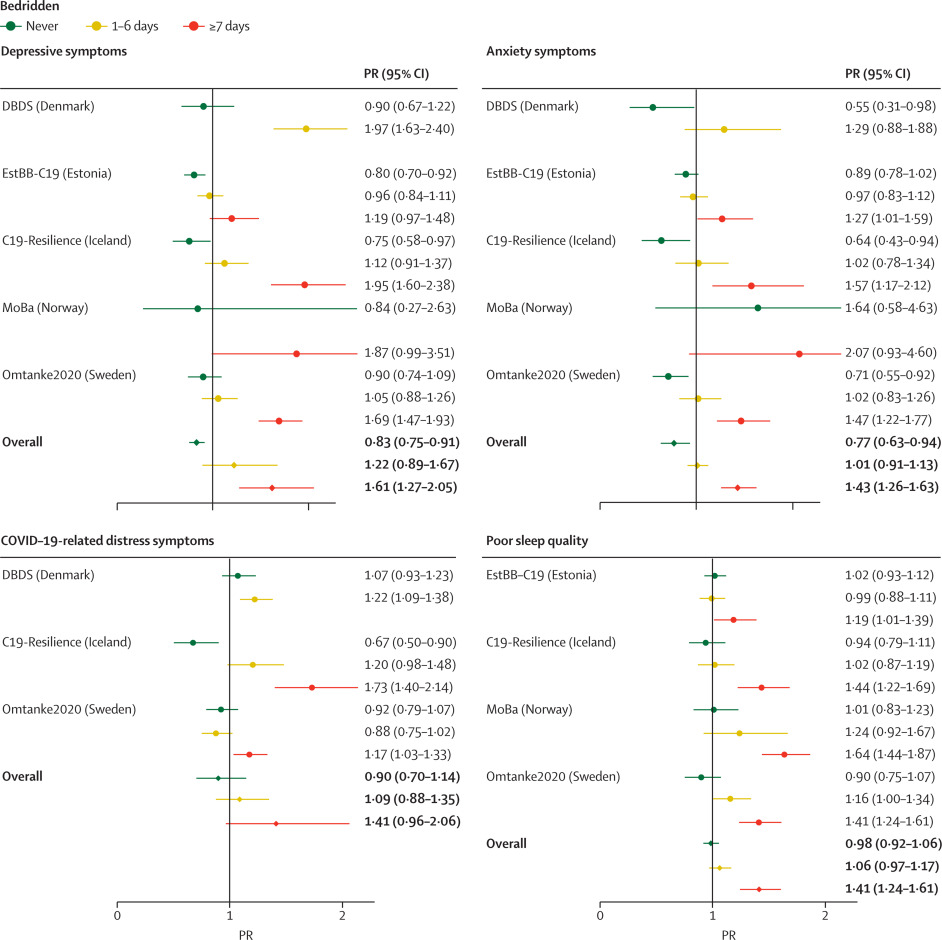
Findings. The analytical cohort consisted of 247 249 individuals, 9979 (4·0%) of whom were diagnosed with COVID-19 during the study period. Mean follow-up was 5·65 months (SD 4·26). Participants diagnosed with COVID-19 presented overall with a higher prevalence of symptoms of depression (prevalence ratio [PR] 1·18 [95% CI 1·03–1·36]) and poorer sleep quality (1·13 [1·03–1·24]) but not symptoms of anxiety (0·97 [0·91–1·03]) or COVID-19-related distress (1·05 [0·93–1·20]) compared with individuals without a COVID-19 diagnosis. Although the prevalence of depression and COVID-19-related distress attenuated with time, individuals diagnosed with COVID-19 but never bedridden due to their illness were consistently at lower risk of depression (PR 0·83 [95% CI 0·75–0·91]) and anxiety (0·77 [0·63–0·94]) than those not diagnosed with COVID-19, whereas patients who were bedridden for more than 7 days were persistently at higher risk of symptoms of depression (PR 1·61 [95% CI 1·27–2·05]) and anxiety (1·43 [1·26–1·63]) than those not diagnosed throughout the study period.
Interpretation. Severe acute COVID-19 illness—indicated by extended time bedridden—is associated with long-term mental morbidity among recovering individuals in the general population. These findings call for increased vigilance of adverse mental health development among patients with a severe acute disease phase of COVID-19.
Corresponding authors:
Ingibjörg Magnúsdóttir and Unnur Anna Valdimarsdóttir
Center of Public Health Sciences, Faculty of Medicine, University of Iceland

